Growth Hormone as Treatment For Fibromyalgia
By Lisa Wells, RN

In the 26 years I have been involved with human growth hormone (GH or HGH) therapies I have many times been asked whether it helps those who suffer with fibromyalgia. Over these past years I have heard clients diagnosed with fibromyalgia who have reported improvements with their symptoms while taking growth hormone therapy.
The Growth Hormone and IGF-1 Factor
Clinical studies have found a correlation between patients with fibromyalgia and low blood IGF-1 levels. The growth factor IGF-1 (insulin-like growth factor #1) is released by the liver in response to the release of growth hormone by the pituitary gland. Because of this fact patients with low IGF-1 levels usually have low GH.
According to Dr. Kevin Yuen many fibromyalgia patients also have low serum growth hormone levels with the hypothesized cause being a dysregulation of the GH/IGF-1 axis.1
In a clinical study done by Kevin C.J. Yuen, Robert M. Bennett, Cheryl A. Hryciw, et al., the researchers found that a subpopulation of fibromyalgia patients who have low serum IGF-I levels will fail the GHRH-arginine test. This testing uses infusions of GHRH (growth hormone releasing hormone) and the amino acid arginine in order to stimulate the pituitary gland to release growth hormone. For this reason they recommended that the GH reserve of these patients should be evaluated further, since restoring their growth hormone to a more healthy level may improve their symptoms.1
Test Subjects Saw Improvements
In a year long study done by G. Cuatrecasas, C. Riudavets, MA Guell, and A. Nadal the group receiving growth hormone received a 60% reduction in their tender points compared to the control group. Similar improvements were observed in the GH group in regards to the Fibromyalgia Impact Questionnaire (FIQ score) compared to the control group. Improvements began to be seen within the first months in most cases. Studies of the test subjects found that symptoms decreased substantially with the increase of their previously low IGF-1 levels.2
In another study done by RM Bennett, SC Clark, and J. Walczyk a group of fifty women with fibromyalgia and low IGF-1 levels were enrolled in a randomized, placebo-controlled double-blind study of nine months duration. These patients gave themselves daily subcutaneous injections of either growth hormone or placebo. Improvements were reported within the first six months of GH therapy with significant improvements being seen after nine consecutive months of GH therapy. After the study, when the growth hormone therapy was discontinued, the test subjects reported a worsening of their symptoms.3
Restoring Low GH and IGF-1 Levels
Improvements in symptoms have been reported by patients taking synthetic growth hormone injections and also by patients taking non-injection products to help improve their GH and IGF-1 levels.
As previously stated, through the years I have heard many positive reports from clients taking our HGH Plus IGF-1 & IGF-2 product. If you would like to learn more please see the top menu.
The Mystery of Fibromyalgia
Fibromyalgia is defined as pain in the fibrous tissue of the body. It has been around for a long time, yet in the past it was often misdiagnosed as rheumatoid arthritis, hypothyroidism, chronic fatigue syndrome, or giant cell arteritis. It is not life threatening, it is a chronic disease. We do not know the exact cause and it cannot be diagnosed by the usual medical tests such as blood studies, X-rays, MRI's, CT scans, etc.
Between three to six million Americans presently suffer with fibromyalgia. It is much more common in women than in men by a ratio of 20:1. The onset typically occurs between the ages of 29 and 37, although it can strike at any age.
As a registered nurse and also a past sufferer of fibromyalgia I have witnessed an opinion by some in the medical profession that the idea and symptoms of fibromyalgia are in the patient's head.
In the medical community some have had the opinion that some physicians will diagnose a patient as having fibromyalgia when the physician cannot find medical evidence of any other illness. Some believe the doctors do this partly to satisfy the patient by giving him/her a specific diagnosis.
Fibromyalgia is now finally getting more attention in the medical profession as a legitimate diagnosis but there are still some who have the opinion that since it is not life threatening and cannot be diagnosed by traditional means, and because it is chronic the patient must learn to live with it. Thankfully, we are now moving away from that way of thinking and are now giving patients with fibromyalgia the attention and concern they deserve.
Possible Physiologic Causes of Fibromyalgia
Human Growth Hormone: Is needed for homeostasis and rejuvenation, is primarily secreted during deep sleep. Studies show a tendency for fibromyalgia patients to have low IGF-1 and GH levels.
Nutritional Deficiencies: There is new evidence to support the thought that deficiencies of magnesium may play an important role, and vitamin D and folic acid are receiving attention. Some studies have also shown that deficiencies in serotonin precursors such as tryptophan may be a cause.
Disruption in Restorative Deep Sleep: Serotonin is needed for deep sleep, when it is depleted the patient has less deep rejuvenating sleep.
Altered Microcirculation in Muscle Tissue: This may contribute to muscle hypoxia and ischemia, causing the fatigue, muscle tenderness, and pain patients experience 24 to 48 hours after exercise.
Increased Pain Perception Due to an Increase in Substance P: Substance P is a neuropeptide that carries pain signals. It helps nervous system cells communicate with each other about painful stimuli. An increased level of substance P leads to increased pain perception. A study found that fibromyalgia patients have less blood flow to two areas of the brain that regulate the amount of pain signals received by the brain, giving them less ability to control pain.
Physical or Emotional Trauma: Some patients report symptoms beginning after physical or emotional trauma, such as a motor vehicle accident, divorce, or death of a loved one.
Genetics: It may be familial in nature. Studies show that a high prevalence of patients have family members with the disease, particularly mothers (83%), sisters (63%), and daughters (26%). Interestingly, 19% of patients have husbands who also have fibromyalgia, indicating a possible environmental, dietary, or lifestyle component.
Depression: This is a chicken or egg issue, does depression cause fibromyalgia or does fibromyalgia cause depression?
Diagnosing Fibromyalgia
As stated above, it is usually diagnosed by ruling out other conditions such as rheumatologic syndromes, hypothyroidism, etc., and by obtaining an accurate and detailed patient history.
The American College of Rheumatology
Fibromyalgia Diagnostic Guidelines and Criteria
Pain in the upper and lower body bilaterally and on the spine and persisting for three or more months.
Pain on palpation in at least 11 of the 18 tender points.
Anterior Tender Points
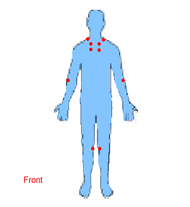
Posterior Tender Points
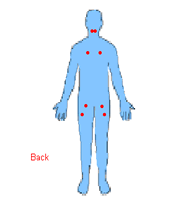
The Patient May Suffer With Some of the Following Symptoms:
Stiffness exacerbated by inactivity
Swelling in the soft tissues
Muscle spasms and/or palpable nodules in affected muscles
Mood swings and depression
Difficulty with memory and concentration
Paresthesia
Hypoglycemic-like syndrome
Irritable bowel or bladder syndrome
Headaches
Chronic fatigue and decreased endurance
Sleep disturbances and the inability to obtain deep level sleep
Dysmenorrhea
Chronic pelvic pain in women
Disequilibrium
Environmental sensitivity
Common Treatments For Fibromyalgia
Pharmacological Therapy
Mainstream medical doctors may prescribe pharmaceutical drugs.
Medications such as duloxetine (Cymbalta), milnacipran (Savella) and pregablin (Lyrica) are FDA approved for treatment of fibromyalgia.
Anti-anxiety drugs and antidepressants such as tricyclics and selective serotonin re-uptake inhibitors (SSRI) are commonly used.
Some prescribe zolpidem (Ambien) and alprazolam (Xanax) as short-term sleeping aids.
Muscle relaxants and NSAIDs may be prescribed for muscle spasms and to control pain.
Local anesthetics or corticosteroid injections at painful tender points are other options.
Opiate analgesics may be used when pain is moderate to severe despite other therapies.
Exercise Therapy
Once the patient gets over the initial pain hurdle, one of the most beneficial treatments is exercise.
Exercise increases endorphins, the body's natural painkillers and sleep-deepening substances and stimulates the secretion of human growth hormone, serotonin, and blood flow to the muscles.
A physician who specializes in physical medicine and rehabilitation should recommend and design a program tailored to the patient's condition. For example, the patient may begin with just three to five minutes of exercise per day with slow increases to avoid inducing pain.
Swimming or exercising in water is often recommended because it puts less strain on the joints. The patient's muscles may have atrophied from prolonged inactivity. Collaborating with a physiatrist should give the patient the support needed to build up stamina.
Other Therapies
IGF-1 restoration through growth hormone therapy may improve symptoms substantially.
Nonpharmacologic treatments include cognitive therapy and psychotherapy which can help patients understand and deal with the pain and life changes brought about by fibromyalgia.
Massage therapy can help with general muscle aches and pains and stretching can help limber up inactive joints.
Acupuncture can be combined with other therapies for pain relief.
Because symptoms change over time treatment is progressive and should be individually tailored to the patient.
Bibliography
1. Kevin C.J. Yuen, Robert M. Bennett, Cheryl A. Hryciw, Marie B. Cook, Sharon A. Rhoads, David M. Cook, Is further evaluation for growth hormone (GH) deficiency necessary in fibromyalgia patients with low serum insulin-like growth factor (IGF)-I levels?, Growth Hormone & IGF Research, Volume 17, Issue 1, 2007, Pages 82-88, ISSN 1096-6374, doi: 10.1016/j.ghir.2006.12.006
2. Cuatrecasas G, Riudavets C, Guell MA, Nadal A. Growth hormone as concomitant treatment in severe fibromyalgia associated with low IGF-1 serum levels. A pilot study. BMC Musculoskelet Disord. 2007 Nov 30;8:119. doi: 10.1186/1471-2474-8-119. PMID: 18053120; PMCID: PMC2212629
3. Bennett RM, Clark SC, Walczyk J. A randomized, double-blind, placebo-controlled study of growth hormone in the treatment of fibromyalgia. Am J Med. 1998 Mar;104(3):227-31. doi: 10.1016/s0002-9343(97)00351-3. PMID: 9552084
4. Wolfe F, Clauw DJ, Fitzcharles MA, Goldenberg DL, Katz RS, Mease P, Russell AS, Russell IJ, Winfield JB, Yunus MB. The American College of Rheumatology preliminary diagnostic criteria for fibromyalgia and measurement of symptom severity. Arthritis Care Res (Hoboken). 2010 May;62(5):600-10. doi: 10.1002/acr.20140. PMID: 20461783


